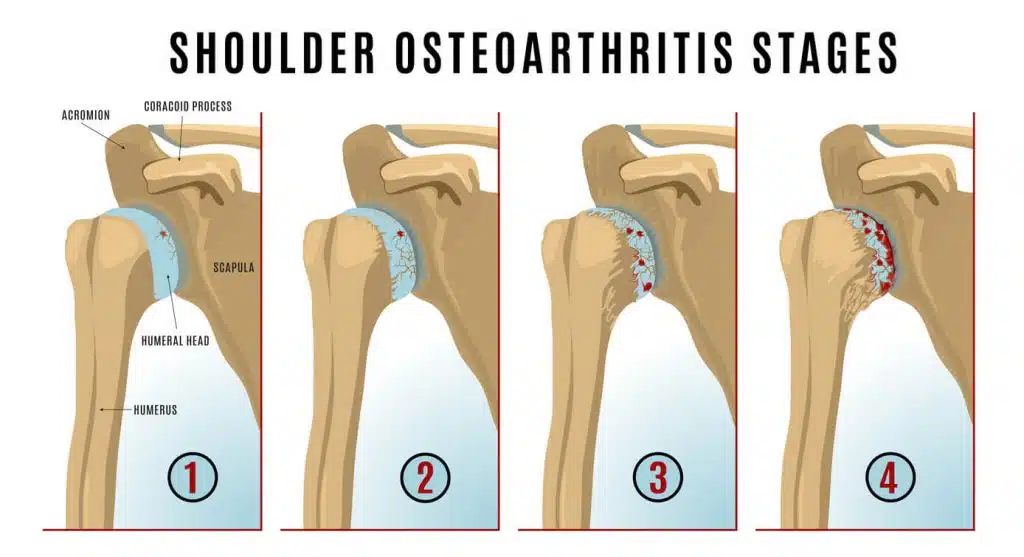
Shoulder osteoarthritis affects a significant number of people, especially as they age. It’s a type of arthritis that occurs in the shoulder joint, causing pain, stiffness, and a reduction in the range of motion. In this article, we’ll delve into what shoulder osteoarthritis is, how it impacts daily life, and the surgical treatment options you can consider.
Whether you’re a patient dealing with this condition or someone looking to understand more about it, this article will help you navigate the path toward better shoulder health.
1. Arthroscopy for Shoulder Osteoarthritis
Arthroscopy is a minimally invasive surgical procedure that’s often considered for treating certain types of shoulder osteoarthritis. It is typically considered for patients experiencing the early stages of the condition.
This technique involves making small incisions around the shoulder and inserting a tiny camera, known as an arthroscope, into the joint.
This camera displays images on a screen, allowing the surgeon to guide miniature surgical instruments to repair or remove damaged tissues.
The Procedure
The procedure typically lasts one to two hours and is usually done under general anesthesia.
The surgeon will make small incisions around the shoulder, through which the arthroscope and surgical instruments are inserted. They then carefully:
- Examine the joint
- Identify any damaged areas
- Perform necessary repairs
This might include trimming or repairing torn cartilage, removing bone spurs, or releasing tight ligaments.
Recovery and Outcomes
Recovery from arthroscopy is generally quicker than open surgery. Patients often return home the same day and begin physical therapy soon after.
Most people experience a significant reduction in pain and improvement in joint function.
However, the extent of recovery and the time it takes vary depending on the specific procedure and the individual’s overall health.
Following post-operative instructions and engaging in recommended rehabilitation exercises is crucial for optimal recovery.
2. Shoulder Joint Replacement
Shoulder joint replacement is typically considered for severe shoulder osteoarthritis, where the joint is significantly damaged and other treatments have not provided relief.
This procedure involves replacing the damaged parts of the shoulder joint with artificial components.
Types of Shoulder Replacements
- Total Shoulder Arthroplasty: Involves replacing both the ball (humeral head) and the socket (glenoid) of the shoulder joint.
- Partial Shoulder Replacement: Only the ball of the joint is replaced.
- Reverse Total Shoulder Replacement: The positions of the ball and socket are switched, which is particularly useful in cases with damaged rotator cuffs.
Procedure and Recovery
The surgery is performed under general anesthesia and typically takes a few hours. The surgeon:
- Makes an incision over the shoulder
- Removes the damaged parts of the joint
- Replaces them with the prosthetic components
After the surgery, the patient stays in the hospital for a short period to be monitored.
Recovery involves a stay in the hospital, followed by several weeks of rehabilitation. Physical therapy is crucial and starts soon after surgery to maintain motion and strength in the shoulder.
Full recovery and a return to normal activities can take several months. Most patients experience significant pain relief and improved function in the replaced shoulder.
Regular follow-ups with the surgeon are essential to monitor the progress and longevity of the implant.
Evaluating the Need for Surgical Intervention
Deciding to undergo surgery for shoulder osteoarthritis is a significant step that should be considered carefully. Surgery is typically advised when non-surgical treatments have not provided adequate relief and quality of life is severely impacted.
Here are key factors to consider:
1. Severity of Symptoms
If you experience intense pain, stiffness, and limited mobility that interferes with daily activities, work, or sleep, surgery may be the next step.
2. Response to Non-Surgical Treatments
Surgery is often considered when pain medications, physical therapy, and lifestyle modifications fail to alleviate symptoms effectively.
3. Joint Damage
Severe joint damage seen in imaging tests like X-rays or MRIs, especially when there’s significant cartilage loss or bone damage, often necessitates surgical intervention.
4. Lifestyle and Activity Levels
If your lifestyle or work requires significant shoulder mobility that you can no longer achieve due to osteoarthritis, surgery might be necessary to restore this function.
5. Patient’s Overall Health
Good candidates for surgery are generally in good health, with no underlying conditions that would increase the risk of surgery. Age, though a factor, is not the sole determinant.
6. Patient’s Expectations
It’s important for patients to have realistic expectations regarding the outcomes of surgery, including the recovery process and the potential for improved mobility and pain relief.
7. Surgeon’s Recommendation
A surgeon’s assessment, based on a comprehensive evaluation of your condition, is crucial in deciding if surgery is appropriate and which type of surgery would be most beneficial.
High-Quality Shoulder Surgery in Catonsville, MD
Shoulder osteoarthritis can be a challenging condition, but there are many paths to relief and recovery. From understanding the basics of the condition to weighing the pros and cons of various surgical options, it’s all about making informed choices. The decision to undergo surgery is personal and should be made in consultation with a qualified provider. With the right information and support, you can look forward to improved mobility and a better quality of life.
You can depend on Orthopaedic Associates of Central Maryland for personalized and effective treatment of shoulder pain in Baltimore. Under our care, you can rest assured you will receive nothing short of the best services, which you deserve. Book a visit with the top practice of orthopedics in Baltimore through our online appointment request form. You may also call (410) 644-1880 for assistance.
We look forward to serving you!


